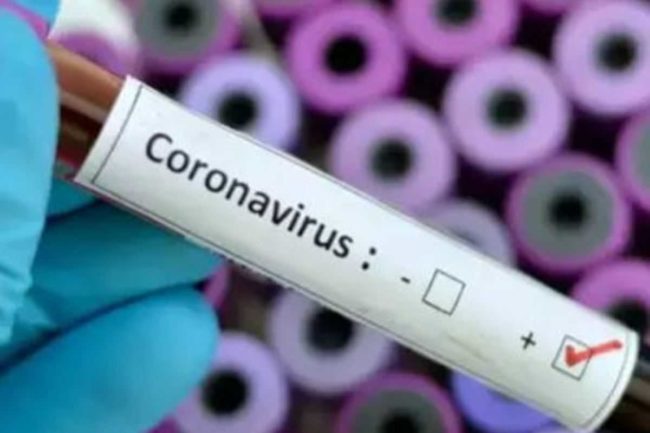
With ‘in a research minute’, I have no choice but to address the impact of the Coronavirus to clinical trials. So here we go.
Although in the grand scheme of things, the impact to clinical trials may not be the world’s first concern, there are still significant patient safety considerations to be made. As this is a fast-developing situation, it may well be that I find myself needing to update this blog post. When this occurs, I’ll add update notes underneath this post, to indicate what changed.
It is only 10 days ago that Barrons reported on the responses of drug companies to the pandemic1. Verbally, it was clear that the companies are worried, but officially no drug companies expressed concern in statements to Barron’s. Bristol-Myers Squibb said it had seen no impact to its clinical trials at this time. Merck said it did “not believe” that any of its “global studies are at risk.”
I wonder what the current thinking on that is. Because I think this was even at that time an underestimation of the impact of this crisis on clinical trials. Sponsors should expect data quality issues due to missed visits and a reduction in enrolment rates. Investing in patient engagement initiatives and coordinating directives with study sites should help with mitigating risks caused by the Coronavirus disruption2.
 Sponsor companies and CROs will currently be scrambling to work out how to mitigate the impact of this outbreak, and if they’re not, they should be. And at least, they should be communicating to sites and responding to questions. I have already heard sites indicating that there is a clear lack of (consistent) communication from the sponsors and the CROs.
Sponsor companies and CROs will currently be scrambling to work out how to mitigate the impact of this outbreak, and if they’re not, they should be. And at least, they should be communicating to sites and responding to questions. I have already heard sites indicating that there is a clear lack of (consistent) communication from the sponsors and the CROs.
In areas where the healthcare system is starting to get overloaded as a result of the outbreak, there will be less time and attention to trial visits. And even where the sites are not (yet) overloaded, visiting the sites for trial visits could be considered an additional risk to the subjects, as they’ll be attending hospitals and clinics for those, where the risk of exposure may well be higher.
The best situated, at this point, are dedicated research centres. They will be able to schedule such that the subjects will not have to wait in crowded waiting rooms and they’ll be better able to take precautionary measures for the protection of the subjects.
The current situation is not likely to get better soon and even most likely will get worse for the foreseeable future. Larger parts of the world’s population are going into either enforced isolation or self-quarantine. And, although not everywhere in the world, in many places subjects will have a harder time to make their visits on time, or in person.
It may not always be clear for sites what would currently be the best way to handle the situation. Guidance from the sponsors and CROs is needed. There are a number of safety and ethical considerations.
The safety considerations are direct to trial subjects. They are both trial-related (Will a missed visit result in missing safety assessments? Will subjects be able to obtain their next treatment doses in time?) and non-trial related (Will trial visits increase the risk of exposure for the subjects?) Fear of the virus and travel restrictions are currently also non-trial related factors2.
Ethical considerations exist on a higher trial level. Trials cannot afford to lose protocol visits to the extent that the evaluability of the trial becomes a risk. With the efforts that the participating subjects are making and the inherent risks to trial participation, it is unethical to end up with trial results that are not suitable for analysis.
Although I expect that the regulatory authorities will not enforce penalties for trials that fail to meet their endpoints as a result of the outbreak, it can be expected from sponsors that they are able to demonstrate efforts made to prevent this situation from happening.
 By now, regulatory authorities are starting to issue guidance for the management of clinical trials in relation to the coronavirus. The MHRA (UK) 3 indicates that prospective protocol waivers remain unacceptable. That said, however, there could still be actions taken to eliminate immediate hazards to subjects. This may include actions to reduce potential exposure to COVID-19, or to continue to provide medically necessary study care (including study drug) to participants who have been placed in isolation or quarantine because of suspected or known exposures.
By now, regulatory authorities are starting to issue guidance for the management of clinical trials in relation to the coronavirus. The MHRA (UK) 3 indicates that prospective protocol waivers remain unacceptable. That said, however, there could still be actions taken to eliminate immediate hazards to subjects. This may include actions to reduce potential exposure to COVID-19, or to continue to provide medically necessary study care (including study drug) to participants who have been placed in isolation or quarantine because of suspected or known exposures.
The FDA has issued ‘Guidance on Conduct of Clinical Trials of Medical Products during COVID-19 Pandemic‘3a. It provides general guidance, focussing as expected on the protection of the trial subjects and the data integrity. Their conclusion: “Robust efforts by sponsors, investigators, and IRBs/IECs to maintain the safety of trial participants and study data integrity are expected, and such efforts should be documented. […] FDA recognizes that protocol modifications may be required, including unavoidable protocol deviations due to COVID-19 illness and/or COVID-19 control measures. Efforts to minimize impacts on trial integrity, and to document the reasons for protocol deviations, will be important.”
If a sponsor or investigator needs to make a change to a protocol in order to eliminate apparent immediate hazards to subjects, these changes can be made and then reported to the IRB/IEC as soon as possible after the fact4.
The least of the worries of clinical trials, at this point, should be quality control. Of course, I’m aware of the impact that this current crisis has on a lot of companies and perhaps even more so on freelancers working in clinical research, I’m currently addressing the impact of the coronavirus to subjects and trial management.
In areas where a travel restrictive advice is in place, monitoring visits should be halted. Where the overall population is instructed or advised to restrain from getting together in groups larger than a particular number, monitors should no longer go to sites. Quite often, sites will already cancel visits for non-medical reasons, but sponsors and CROs should take their responsibility pro-actively and not add unnecessarily to the burden of the health care systems. Sites deliver quality. And where they need their attention to focus on medical care and performing trial visits from subjects, quality control can wait until all this has come to rest.
The ACRO (Association of Clinical Research Organisations) published “Considerations to Support Clinical Trial Monitoring Oversight During COVID-19“4a. These are considerations for then on-site monitoring is no longer possible, using remote monitoring options, taking care not to put any extra burden on clinical trial sites.
The ACRO is also providing considerations on how to proceed when on-site monitoring can be resumed, and considerations for when the scheduled database lock is before resuming on-site monitoring focussing on a risk-based approach.
The FDA has announced that they are postponing foreign inspections through April 5. I fully expect all other regulatory authorities to take a reasonable approach to inspections at this time as well. The same goes for audits. Myself, I’m seeing audits being postponed until a later time. And this is the kind of actions that are currently justified.
Overall, let’s prioritise as much as we can. First, obviously, medical care for all takes priority over trial visits. That said, continuing trial visits are in many cases quite important for the participants as they need their continued care and medication. Where possible, certain trial-related actions can perhaps be done remotely? Efforts need to be made to ensure as much as possible that clinical trials remain evaluable.
And more than before, this current crisis illustrates the need for clinical trials to embrace decentralisation of trials where that would be possible. A hybrid approach to clinical trials is a topic that’s becoming more current by the day. However, for now, that’s a topic for another time.
Before finishing this post, let me give a shout-out to Vincent Bontrop, who in his (Dutch languaged) blog post6 provides a wonderful overview of (inter)national guidances. Even if you’re not Dutch-speaking, it may well contain useful links to guidance from countries you work in or with.
Let me finish here with a heart-felt Stay Safe. Take care of yourselves as well as your trial subjects. Because in crises like this, situations can change in a research minute.
UPDATES:
18 March: Included FDA guidance and ACRO guidance.
18 March: Included reference to a blog post from Vincent Bontrop
2 http://www.appliedclinicaltrialsonline.com/clinical-trials-feel-coronavirus-crunch
3a https://www.fda.gov/media/136238/download
4 https://www.clinicalleader.com/doc/changes-to-research-made-in-response-to-covid-0001
6 https://blog.bontrop.com/2020/03/coronavirus-covid-19-clinical-research-een-overzicht/